Psychotherapy Outcome for College Students with ASD and other Disabilities in a National Sample: Replication, Refinement, and Extension
The April 2022 CCMH blog post has been guest authored by Jonathan C. Cox and E. Shannon Neeley-Tass at Brigham Young University, Provo, UT. Dr. Cox and Dr. Tass have graciously written April's post to share their findings for Autism Acceptance Month. CCMH is incredibly grateful to Dr. Cox and Dr. Neeley-Tass for conducting this important research, using the CCMH dataset, and for share their findings with the CCMH community.
Introduction
College and university counseling centers (UCC) provide mental health services for a wide range of difficulties and populations, including students with various disabilities. A subset of this population of students seeking mental health services are those with Autism Spectrum Disorder (ASD). Young adults with ASD often experience high rates of comorbid mental health concerns. Unfortunately, a majority of these UCCs do not provide services that are specifically geared towards individuals with ASD. Furthermore, few studies have investigated the effectiveness of standard psychotherapeutic care provided in UCCs for young adults with ASD.
In 2017, we examined the therapy outcomes of students with ASD at one UCC compared to their peers at the same center (Anderberg et al., 2017). We discovered that they experienced equivalent amounts of change as their peers; however, students with ASD participated in significantly more sessions than their peers.
In contrast to our results, O’Shea and colleagues (2021) examined the therapy outcomes of a much larger sample of college students with many different types of disabilities, including ASD. Using a large, national sample from 112 UCCs, they reported that students with disabilities experienced less improvement in counseling than their peers who reported no disability. They indicated that improvement in counseling may depend somewhat on the type of disability a student experiences. They reported that in their study, clients with a physical disability may have experienced less change on a measure of academic distress than clients with a psychiatric disability. However, this between-groups difference, although noticeable, was not statistically significant. O’Shea and colleagues called for more detailed research focusing on the therapy outcomes of populations with different disabilities and presenting concerns.
We attempted to answer this call by examining how individuals with ASD fared in psychotherapy, including treatment length and treatment outcome, at UCCs in the U.S. compared to peers of differing disability statuses and peers with no reported disability. The following research questions were answered:
- Do students with ASD and other disabilities attend significantly more or less sessions of therapy than their peers who report no disabilities?
- Do students with ASD and other disabilities benefit as much from therapy as their peers who report no disabilities?
Method
We used a national CCMH data set containing information on 178,486 clients that visited 124 college and university counseling centers (UCC) during the 2015-2016 and 2016-2017 academic years. We compared students who indicated on their intake documentation that they have been diagnosed with ASD with their peers who reported other disability statuses and with peers who reported no disability at intake.
Measures
Students who request services from a UCC are frequently asked to complete the Standardized Data Set (SDS) at their initial appointment. On the SDS, students are asked to report their status on a number of demographic variables that are common in the research literature, including age, gender, ethnicity, academic status, disability status, etc.; as well as elements of their psychiatric history. Data from the SDS were used to divide the sample into the groups compared in this study.
Students who receive services from a UCC are also frequently asked to complete a measure of psychological distress, the Counseling Center Assessment of Psychological Symptoms (CCAPS), at their initial session of counseling and at repeated measures during treatment. The CCAPS has seven subscales: depression, generalized anxiety, social anxiety, academic distress, eating concerns, alcohol use, hostility, and a measure of general psychological distress (Distress Index, DI).
We divided the data (n = 178,486) into four groups who reported different types of disabilities:
- ASD (n = 867)
- Physical Disabilities (n = 2,431)
- Psychological Disabilities (e.g. Depression, Anxiety, etc.; n = 10,568)
- Other Disabilities (e.g. Learning Disabilities, ADHD, etc.; n = 2,480)
- No Disabilities (n = 162,140)
Results
Treatment Length
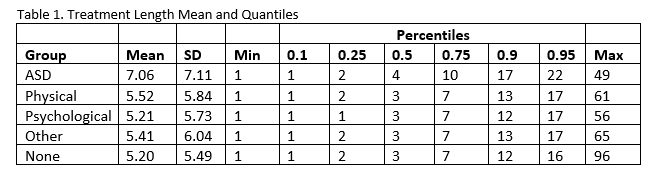
We examined treatment length using quantile regression for the number of sessions attended, similar to Anderberg et al. (2017). Students with ASD attend, on average, about 1.5 more sessions than their peers with other disabilities and no disabilities. Further, the quantile regression indicated that students in the higher percentiles of the ASD group (i.e. students within this group who attended the most sessions) attended significantly more sessions than the students in the Physical, Psychological, and No Disability groups from the same quantile (see Table 1). For example, the 25% of students with ASD who attended the most sessions had an average of 10 sessions, while the top 25% of students within other groups attended an average of 7 sessions, and the differences become more pronounced at higher percentiles.
Treatment Outcome
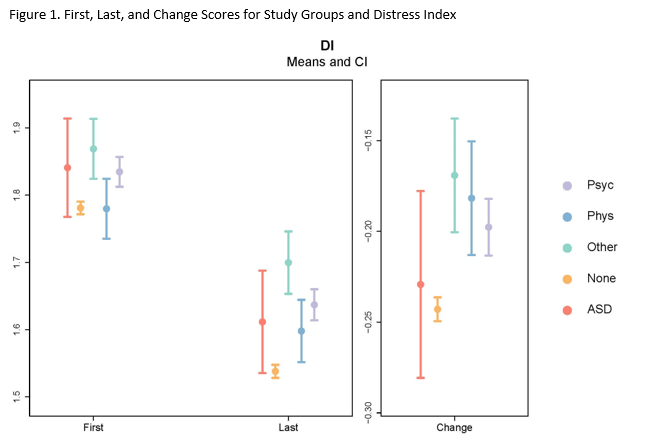
To investigate treatment outcomes, we compared students with ASD, physical disabilities, psychological disabilities, other disabilities, and no disabilities on their first CCAPS scores, last CCAPS scores, and their CCAPS change (with negative change indicating improvement) for each subscale and the DI (Distress Index). There were numerous differences between the four groups in terms of amount of change across several areas of distress, including overall distress (DI). Differences on the DI are illustrated in Figure 1 as an example, with results from other subscales described in the text.
Students with ASD, on average, demonstrated similar levels of change in counseling compared to their peers with other disabilities and those with no disability. Students in the no disability group demonstrated significantly more change than students in the psychological, physical, and other disabilities groups on the Distress Index (see second panel in Figure 1). Interestingly, students with ASD exhibited a lot of variability in their change scores, as indicated by the wide confidence interval band in Figure 1. A similar pattern of results were found for the depression, generalized anxiety, and social anxiety subscales.
Students in the ASD group and the no disabilities group demonstrated significantly more change than the students in the other disabilities group on the hostility subscale. Conversely, students in the psychological and no disabilities groups demonstrated significantly more change than students in the ASD, physical, and other disabilities groups on the alcohol use subscale.
Additionally, students in the no disability group demonstrated significantly more change than students in the physical and other disabilities groups on the academic distress subscale, while students in the psychological disability group demonstrated significantly more change than students in the other disabilities group on the academic distress subscale. Finally, students in the no disabilities group demonstrated significantly more change than students in the psychological and other disabilities groups on the eating concerns subscale.
Overall, students with ASD appear to experience similar levels of change from counseling as their peers on the DI and most subscales, while experiencing significantly more change on the hostility subscale, and significantly less change on the alcohol use subscale.
Discussion
In this study, we tested the generalizability of the results we described in Anderberg et al. (2017) for college students with ASD who engaged in counseling at one university, as well as extended the findings of O’Shea and colleagues (2021) regarding students reporting differing disability statuses who engaged in counseling at UCCs. Our results indicate that students with ASD in a nationwide sample appeared to engage in significantly more therapy sessions than their peers. Additionally, students with ASD tend to demonstrate similar levels of change on the CCAPS, a measure of symptoms distress, compared to their peers with no reported disability.
Furthermore, our findings also replicate, refine, and extend the results of O’Shea et al. In this study, we demonstrate that individuals with disabilities experience significant change in counseling on different subscales of the CCAPS, depending on the type of disability an individual has reported. For example, students with ASD appear to experience the same amount of change in counseling at UCCs on the DI and most subscales of the CCAPS as their peers who report no disabilities. It may be that students with different disabilities experience distress due to different ways that their disabilities impact their functioning. Because of the complexity of the various differences between groups in this study, we recommend that future research investigate the reasons that students with different disability types benefit from therapy in different ways. We hope that our research can help UCCs to begin to look at more tailored treatment and services for students with different disability types.
Limitations
One of the major limitations of this study is due to the variable and inconsistent policies of measurement at different UCCs. Because different centers collect data at different timeframes, the sample sizes of students with usable data for some of the disability groups, especially students with ASD, were much smaller than we hoped, and decreased the power of our analyses. Further research on ASD clients, and clients with other disabilities, will be increasingly possible as UCCs administer the CCAPS regularly throughout treatment.
References
- Anderberg, E., Cox, J. C., Tass, E. S. N., Erekson, D. M., Gabrielsen, T. P., Warren, J. S., Cline, J., Petersen, D., & South, M. (2017). Sticking with it: Psychotherapy outcomes for adults with autism spectrum disorder in a university counseling center setting. Autism Research, 10(12), 2048–2055. https://doi.org/10.1002/aur.1843
- Center for Collegiate Mental Health (2021). CCAPS User Manual. University Park, PA.
- Hayes, J. A., Locke, B. D., & Castonguay, L. G. (2011). The Center for Collegiate Mental Health: Practice and research working together. Journal of College Counseling, 14(2), 101–104. https://doi.org/10.1002/j.2161-1882.2011.tb00265.x
- O’Shea, A., Kilcullen, J. R., Hayes, J., & Scofield, B. (2021). Examining the effectiveness of campus counseling for college students with disabilities. Rehabilitation Psychology, 66(3), 300–310. https://doi.org/10.1037/rep0000349